Original article
Work-related mental disorders in Bahia: an epidemiological analysis from 2013 to 2023 / Transtornos mentais relacionados ao trabalho na Bahia: uma análise epidemiológica de 2013 a 2023
Bárbara Costa Proença1 (https://orcid.org/0009-0008-5199-0821)
Simone Cardoso Passos2 (https://orcid.org/0000-0002-6467-8211)
1C orresponding contact. Escola Bahiana de Medicina e Saúde Pública (Salvador). Bahia, Brazil. [email protected]
2Escola Bahiana de Medicina e Saúde Pública (Salvador). Bahia, Brazil.
ABSTRACT | OBJECTIVE: To analyze the epidemiological profile of work-related mental disorders in Bahia from 2013 to 2023. METHODS: An ecological study with a time-series design, based on secondary data extracted from the Notifiable Diseases Information System - SINAN (Sistema de Informação de Agravos de Notificação). All reported cases of work-related mental disorders registered in the state of Bahia from 2013 to 2023 were included. Data analysis was performed using descriptive statistics. The variables were: sex, race/color, level of education, specific diagnoses, and case evolution. RESULTS: A total of 1654 cases of work-related mental disorders were reported, predominantly among females (1005; 60.5%), individuals aged between 35 and 49 years (923; 55.8%), self-declared mixed-race/brown (581; 35.1%), and those with completed higher education (497; 30.0%). The most prevalent diagnosis was neurotic, stress-related, and somatoform disorders (745; 45.1%), with temporary disability being the most frequent outcome (1163; 70.3%). The results also show a growing trend in the number of cases of work-relat ed mental illness throughout the analyzed period. CONCLUSION: The profile reveals gender and racial inequality, onset in the economically active age group of 35 to 49 years, and an upward trend of work-related mental disorders throughout the analyzed period.
KEYWORDS: Mental Disorders. Working Conditions. Occupational Health.
RESUMO | OBJETIVO: Analisar o perfil epidemiológico dos transtornos mentais relacionados ao trabalho na Bahia no período de 2013 a 2023. MÉTODOS: Estudo ecológico, delineamento de série temporal, baseado em dados secundários extraídos do Sistema de Informação de Agravos de Notificação (SINAN). Foram incluídos todos os casos notificados de transtornos mentais relacionados ao trabalho, registrados no estado da Bahia, no período de 2013 a 2023. A análise dos dados foi realizada por meio de estatística descritiva. As variáveis foram: sexo, raça/cor, nível de escolaridade, diagnósticos específicos e evolução dos casos. RESULTADOS: Foram notificados 1654 casos de transtornos mentais relacionados ao trabalho, com predominância do sexo feminino (1005; 60,5%), idade entre 35 e 49 anos (923; 55,8%), raça/cor autodeclarada parda (581; 35,1%) e com nível superior completo (497; 30,0%). O adoecimento mais prevalente englobou os transtornos neuróticos, relacionados ao estresse e somatoformes (745; 45,1%), apresentando como desfecho mais frequente a incapacidade temporária (1163; 70,3%). Os resultados ainda apresentam uma tendência crescente dos números de casos de adoecimento mental relacionado ao trabalho ao longo do período analisado. CONCLUSÃO: O perfil revela desigualdade de gênero e raça, acometimento da faixa etária economicamente ativa (entre 35 e 49 anos de idade) e aumento da evolução dos adoecimentos por transtornos mentais relacionados ao trabalho ao longo do período analisado.
PALAVRAS-CHAVE: Transtornos Mentais. Condições de Trabalho. Saúde Ocupacional.
How to cite this article: Proença BC, Passos SC. Work-related mental disorders in Bahia: an epidemiological analysis from 2013 to 2023. J Contemp Nurs. 2026;15:e6557. https://doi.org/10.17267/2317-3378rec.2026.e6557
Submitted Nov. 4, 2025, Accepted Mar. 5, 2026, Published Apr. 23, 2026
J. Contemp. Nurs., Salvador, 2026;15:e6557
https://doi.org/10.17267/2317-3378rec.2026.e6557
ISSN: 2317-3378
Assigned editors: Cátia Palmeira, Tássia Macêdo
1. Introduction
Work-related mental disorders (WRMDs) have emerged as a public health problem worldwide, with a particularly pronounced impact in developing countries such as Brazil. Currently, these conditions represent the third leading cause of work absenteeism1.
Since the last decades of the 20th century, the workplace has undergone significant transformations, profoundly altering work environments and conditions. These structural changes have resulted in a reshaped morbidity profile, with an increase not only in workplace accidents but also in occupational diseases, including repetitive strain injuries and mental disorders1,2.
Although the average unemployment rate in Latin America fell from 11.4% in 1999 to 8% in 2007, the main labor-related problems persisted. These included: precarious employment, productivity growth restricted to certain sectors, informal employment, outsourcing of labor, expansion of temporary and informal jobs, low access to social security, reduced severance pay, limitations on the right to strike, and deterioration of income from work1.
In 2004, the Brazilian Ministry of Health, through Ordinance No. 777, included Work-Related Mental Disorders (WRMDs) as a notifiable disease in the Notifiable Diseases Information System (Sistema de Informação de Agravos de Notificação - SINAN) of the Unified Health System (Sistema Único de Saúde - SUS) for all workers, regardless of their employment status3. In 2016, through Ordinance No. 205, the Ministry of Health expanded the monitoring of Work-Related Mental Disorders by including them in the national list of diseases and conditions monitored by the sentinel unit surveillance strategy4.
In Brazil, the National Social Security Institute (Instituto Nacional do Seguro Social - INSS) reports that work-related mental disorders rank third among the main causes for granting social security benefits (sick pay), while the World Health Organization (WHO) estimates that minor mental disorders affect about 30% of workers and more severe mental disorders affect about 5% to 10% of workers5.
WRMDs result from the interaction of multiple factors, ranging from exposure to toxic agents to organizational aspects such as rigid hierarchical structures, long working hours, low wages, multiple jobs, and precarious employment relationships6.
These conditions can trigger psychological distress throughout one's professional life, manifesting as symptoms such as irritability, insomnia, fatigue, difficulty concentrating, decreased performance, and physical complaints7.
Although rarely fatal, these disorders often present a disabling character, significantly compromising productivity, job satisfaction, and quality of life. Furthermore, they present high morbidity and association with other chronic diseases, such as diabetes and cardiovascular diseases. The relationship between work and health is complex and mediated by the psychosocial context; when there is an imbalance between demands and resources available to cope with them, occupational stress emerges as an adaptive response, which can evolve into mental illness8.
This study is justified by the need to understand the epidemiological profile of these health problems in the state of Bahia, in order to contribute to the strengthening of public policies for workers' health, as well as to support strategies for prevention and promotion of mental health in the workplace.
Therefore, the objective of this study is to analyze the epidemiological profile of work-related mental disorders in Bahia from 2013 to 2023.
2. Methodology
This is a cross-sectional, retrospective study with a quantitative approach and a time-series design. The STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) checklist for conducting and reporting the research was used to guide the research.
This study analyzed public data accessed through the TABNET application of the Department of Informatics of the Brazilian Unified Health System (DATASUS). The source used is from the Ministry of Health, specifically the Health Surveillance Secretariat (Secretaria de Vigilância em Saúde - SVS), and registered in SINAN.
Inclusion criteria: The sample included all reported cases of work-related mental disorders registered in the state of Bahia, from 2013 to 2023, according to information available in SINAN. Exclusion criteria: records with individuals under 15 years of age, considering that, according to the Brazilian Institute of Geography and Statistics (Instituto Brasileiro de Geografia e Estatística – IBGE), the minimum legal age for entering the labor market in Brazil is 14 years, exclusively as an apprentice, and 16 years for other forms of work, as established by the Statute of the Child and Adolescent and the Federal Constitution9,10. Therefore, it was decided to exclude age groups under 15 years from the analysis, since they do not correspond to the working population.
Data extraction was performed in February 2025. The variables analyzed were sex, age group, race/color, education level, specific diagnoses available in the system, and the evolution of cases.
The data were organized, structured, and analyzed using Microsoft Excel 2021 software (version 16.0), through the application of descriptive statistics, with the calculation of absolute and relative frequencies.
In accordance with Ruling No. 466/2012 of the National Health Council (Conselho Nacional de Saúde – CNS) since this research uses publicly accessible secondary data and does not individually identify participants, it does not require review and approval by a Research Ethics Committee.
3. Results
There were 1654 reports of work-related mental disorders in Bahia between 2013 and 2023. A predominance of females was observed (n = 1005; 60.5%), among individuals aged 35 to 49 years (n = 923; 55.8%), race/color unknown/blank (n = 642; 38.8%), followed by brown race (n = 581; 35.1%) and those with completed higher education (n = 497; 30.0%).
Table 1. Distribution of reported work-related mental disorders, according to sex, age group, race/color, and education level in Bahia, 2013 to 2023 (n = 1654)
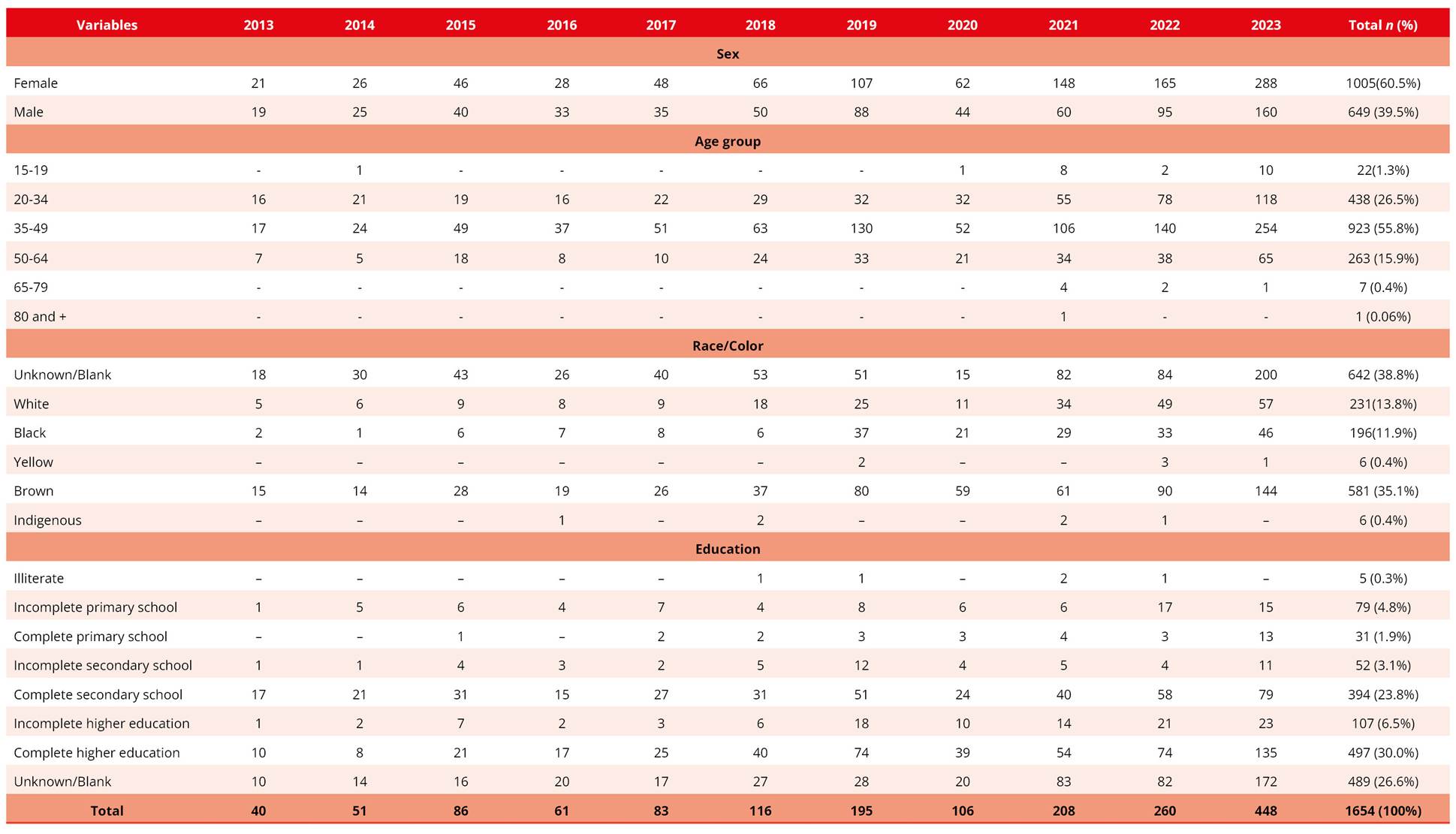
Source: SINAN, 2025.
When analyzing the clinical variables, a predominance of neurotic disorders related to stress and somatoform disorders was observed (n = 755; 45.1%), followed by mood disorders (n = 396; 23.6%). The high proportion of records without ICD codes (n = 171; 10.2%) is also noteworthy (Table 2).
Table 2. Distribution of notifications of work-related mental disorders, according to ICD Diagnosis, in Bahia, 2013 to 2023 (n = 1654)
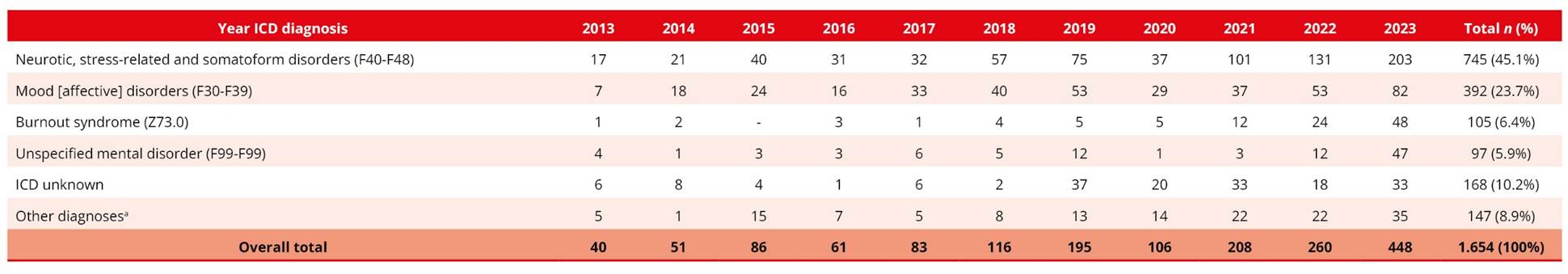
Source: SINAN, 2025.
aIncludes: Other ICDs not listed, Organic mental disorders (F00-F09), Substance use disorders (F10-F19), Schizophrenia and other psychotic disorders (F20-F29), Behavioral syndromes associated with physiological dysfunctions (F50-F59), Personality disorders (F60-F69), Mental retardation (F70-F79), Developmental disorders (F80-F89), Behavioral disorders of childhood/adolescence (F90-F98), Signs and symptoms related to cognition/behavior (R40-R46), Self-inflicted injuries (X60-X84), Social and psychological circumstances (Z55-Z65), Work-related conditions (Y96).
The most frequent outcome was temporary disability (n = 1,163; 70.3%), followed by unknown/blank records (n = 265; 16.0%) (Table 3).
Table 3. Distribution of reported cases of work-related mental disorders according to the evolution of cases in Bahia, 2013 to 2023 (n = 1654)
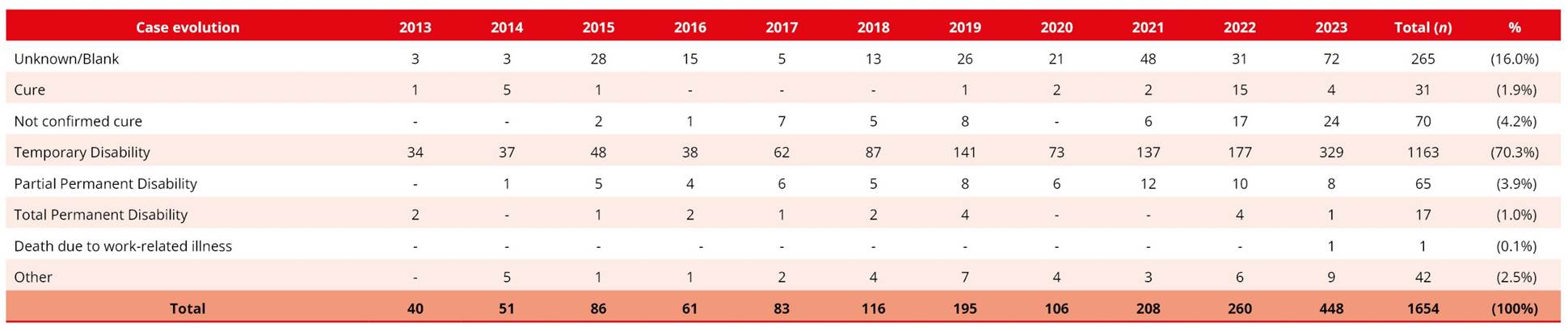
Source: SINAN, 2025.
4. Discussion
The results show that, in Bahia, between 2013 and 2023, WRMDs data was more frequent among individuals with completed higher education, in addition to a significant number of records classified as unknown, which may indicate limitations in the quality of the information.
The analyzed data show an increase in registrations starting in 2019, reaching a peak in 2023. This growth may be related both to the worsening of working conditions, especially after the COVID-19 pandemic, and to the strengthening of epidemiological surveillance and greater awareness among health professionals about the importance of registering these health problems11,12.
The predominance of reported cases among women highlights gender inequalities present in labor relations. Work overload, coupled with domestic responsibilities, double shifts, and professional devaluation, especially in the health, education, and social assistance sectors, increases exposure to psychosocial risks. Evidence indicates that women, particularly Black women, are more vulnerable to disorders such as depression and burnout due to overlapping oppressions and the historical invisibility of their needs. This growing trend in both sexes may be related to increased public awareness, strengthened epidemiological surveillance, and increased reporting by health services in the state of Bahia6.
A cross-sectional study conducted in Bahia, with healthcare workers in municipalities across the state, revealed a significant association between occupational stressors, such as high demands and low autonomy, and common mental disorders, with greater vulnerability among the female population13.
Regarding age group, there was a higher frequency of WRMDs among workers aged 35 to 49. This finding is consistent with the literature, which indicates these age ranges as those with the highest insertion and permanence in the formal labor market, characterized by a high workload, pressure for productivity, and accumulation of functions. Furthermore, the need to reconcile work and family demands increases stress and favors mental illness14. On the other hand, the low reporting rate among adolescents, young professionals starting their careers, and the elderly may be related to lower formal participation in the labor market and underreporting of these groups15.
The analysis of the race/color variable shows a higher frequency of WRMDs among individuals with unknown records and among brown individuals. This finding may reflect, on the one hand, the weakness in completing the race/color category in health information systems, which makes real racial inequalities in health invisible14.
On the other hand, the prominence of mixed-race individuals is consistent with the population composition of Bahia, where most of the population self-identifies as black (both black and brown), groups historically more exposed to precarious working conditions and social vulnerability16.
Regarding education level, there was a higher proportion of notifications among workers with completed secondary and higher education, possibly due to greater access to information and the ability to identify and report symptoms, favoring the seeking of care and the filing of notifications. Studies demonstrate the interrelationship between occupational stressors and gender, race/color, and social class, affecting the mental health of workers17,18.
Regarding outcomes, the predominance of temporary disability shows that, although many workers can return to work after leave, WRMDs have significant impacts on functionality, productivity, and quality of life. The high prevalence of outcomes associated with partial disability or the need for prolonged leave reinforces the severity of these conditions, indicating that a considerable number of workers face substantial functional limitations. These results corroborate a national study that points to mental disorders as one of the main causes of sick leave, generating high economic and social costs14.
Concerning the diagnostic profile, neurotic and stress-related disorders, as well as mood disorders and burnout syndrome, represent the most significant portion of the notifications, highlighting occupational stress as a central factor in mental illness. A meta-analysis study demonstrated that occupational factors such as high stress, workplace harassment, job dissatisfaction, and an imbalance between effort and reward are strongly linked to the development of burnout syndrome19.
The study has limitations that should be considered, namely: 1) the use of secondary data from SINAN implies dealing with a high proportion of unknown/blank fields; 2) the choice of a predominantly descriptive statistical approach did not allow for the exploration of associations between variables; and 3) this is an investigation restricted to a specific region of Brazil, which may limit the generalization of the findings to the country as a whole, given the sociocultural, economic, and epidemiological diversity existing among the different Brazilian regions.
5. Conclusion
The analyzed data revealed a significant occurrence of work-related mental disorders in Bahia, with a predominance of notifications classified as Stress-Related Neurotic Disorders and Mood Disorders. The identified profile points to a pattern of mental illness, especially among workers of working age, women, and people who self-identify as mixed-race, revealing the intersection between work, gender, and race/color in determining psychological distress.
The findings reinforce the need to strengthen worker health surveillance and implement intervention strategies with an emphasis on preventing psychosocial risks and promoting healthier work environments. Furthermore, the importance of considering social markers, such as gender, race/color, education level, and working conditions, in the formulation of public policies is highlighted, since these factors modulate both exposure to occupational stressors and vulnerability to mental illness.
This study contributes to strengthening the evidence base on mental health and work in the context of Bahia, offering support for the formulation of intersectoral policies, the improvement of institutional interventions for worker mental health care, and the development of strategies to reduce underreporting of these conditions, such as training health teams for the proper recognition and recording of cases, integrating information systems, and raising awareness among professionals about the importance of mandatory reporting. Furthermore, the study encourages research that deepens the understanding of health inequalities. The articulation between epidemiological data and theoretical frameworks on social determinants and work organization can support the construction of strategies for care, prevention, and promotion of mental health, reinforcing the urgency of actions to value, protect, and support the working population in the state of Bahia.
Authors’ contributions
The authors declared that they made substantial contributions to the work in terms of the conception or design of the research; the acquisition, analysis, or interpretation of data for the work; and the writing or critical revision of relevant intellectual content. All authors approved the final version to be published and agreed to assume public responsibility for all aspects of the study.
Competing interests
No financial, legal, or political conflicts involving third parties (government, private companies and foundations, etc.) have been declared for any aspect of the submitted work (including, but not limited to, grants and funding, participation on advisory boards, study design, manuscript preparation, statistical analysis, etc.).
Indexers
The Journal of Contemporary Nursing is indexed in DOAJ and EBSCO.
References
1. Franco T, Druck G, Seligmann-Silva E. New labor relations, worker's mental exhaustion, and mental disorders in precarious work. Rev Bras Saude Ocup. 2010;35(122):229-48. https://doi.org/10.1590/S0303-76572010000200006
2. Ministério da Saúde (Brazil), Secretaria de Vigilância em Saúde, Departamento de Análise de Situação de Saúde. Saúde Brasil 2008: 20 anos de Sistema Único de Saúde (SUS) no Brasil [Internet]. Brasília: Ministério da Saúde; 2009. Available from: https://bvsms.saude.gov.br/bvs/publicacoes/sus_20anos_saude_brasil.pdf
3. Portaria no 777/GM, de 28 de abril de 2004 (Brazil). Dispõe sobre os procedimentos técnicos para a notificação compulsória de agravos à saúde do trabalhador em rede de serviços-sentinela específica no SUS. [Internet]. Diário Oficial da União. 2004. Available from: https://bvsms.saude.gov.br/bvs/saudelegis/gm/2004/prt0777_28_04_2004.html
4. Portaria no 205, de 17 de fevereiro de 2016 (Brazil). Define a lista nacional de doenças e agravos a serem monitorados por meio da estratégia de vigilância em unidades sentinelas e suas diretrizes. [Internet]. Brasília: Ministério da Saúde; 2016. Available from: https://bvsms.saude.gov.br/bvs/saudelegis/gm/2016/prt0205_17_02_2016.html
5. Ministério da Saúde (Brazil); Organização Pan-Americana da Saúde no Brasil. Doenças relacionadas ao trabalho: manual de procedimentos para os serviços de saúde [Internet]. Brasília: Ministério da Saúde; 2001. 580 p. (Série A. Normas e Manuais Técnicos; n. 114). Available from: http://bvsms.saude.gov.br/bvs/publicacoes/doencas_relacionadas_trabalho1.pdf
6. Sousa CC, Araújo TM. Combined effects of gender, race, and occupational stressors on mental health. Rev Bras Saude Ocup. 2024;49:edepi12. https://doi.org/10.1590/2317-6369/15222pt2024v49edepi12
7. Cordeiro TMSC, Mattos AIS, Cardoso MCB, Santos KOB, Araújo TM. Reporting of work-related mental disorders among workers in Bahia: a descriptive study, 2007-2012. Epidemiol Serv Saude. 2016;25(2):363-72. https://doi.org/10.5123/S167949742016000200015
8. Fernandes MA, Soares LMD, Silva JS. Work-related mental disorders among nursing professionals: a Brazilian integrative review. Rev Bras Med Trab. 2018;16(2):218-24. https://doi.org/10.5327/Z1679443520180228
9. Presidência da República (Brazil). Lei no 8.069, de 13 de julho de 1990. Dispõe sobre o Estatuto da Criança e do Adolescente e dá outras providências. [Internet]. Diário Oficial da União. Available from: https://www.planalto.gov.br/ccivil_03/leis/l8069.htm
10. Presidência da República (Brazil). Constituição da República Federativa do Brasil de 1988 [Internet]. Senado Federal. Available from: https://www.planalto.gov.br/ccivil_03/constituicao/constituicao.htm
11. Souza SF, Andrade AGM, Carvalho RCP. Mental health and work in the context of the Covid-19 pandemic: proposal for health surveillance. Rev Baiana Saude Publica [Internet]. 2021;45(esp 1):125-39. Available from: https://rbsp.sesab.ba.gov.br/index.php/rbsp/article/view/3242
12. Santos RR. O impacto da pandemia de covid-19 na saúde mental: desafios psicológicos e estratégias de enfrentamento. Rev FT. 2024;29(140). https://doi.org/10.69849/revistaft/ar10202411101011
13. Machado ES, Araújo TM, Sousa CC, Freitas AMC, Souza FO, Lua I. Occupational stress and common mental disorders: how do coping strategies work? Rev Bras Med Trab. 2022;20(2):195-205. https://doi.org/10.47626/1679-4435-2022-680
14. Ministério Público do Trabalho (Brazil), Organização Internacional do Trabalho. Observatório de Segurança e Saúde no Trabalho - SmartLab [Internet]. Brasília: Ministério Público do Trabalho; 2024. Available from: https://smartlabbr.org/sst/
15. Santana AMD, Muñoz D. Notificação de transtorno mental relacionado ao trabalho no Distrito Federal e no território nacional, em 2018 a 2022 – existe subnotificação? Perspectivas [Internet]. 2024;9(supl). Available from: https://www.perspectivas.med.br/2024/11/notificacao-de-transtorno-mental-relacionado-ao-trabalho-no-distrito-federal-e-no-territorio-nacional-em-2018-a-2022-existe-subnotificacao/
16. Fonseca ES, Jorge MA. Discrimination of black women in the labor market: a comparative analysis of income at work in Bahia versus Brazil between 2001 and 2015. Planej Polit Publicas. 2021;(60):265-302. https://doi.org/10.38116/ppp60art9
17. Sousa CC, Araújo TM, Maturino MM. Occupational stressors and mental illness in healthcare work: an intersection between gender, race, and class. Am J Ind Med. 2024;67(2):143-53. https://doi.org/10.1002/ajim.23558
18. Duchaine CS, Aubé K, Gilbert-Ouimet M, Vézina M, Ndjaboué R, Massamba V, et al. Psychosocial stressors at work and the risk of sickness absence due to a diagnosed mental disorder: a systematic review and meta-analysis. JAMA Psychiatry. 2020;77(8):842-51. https://doi.org/10.1001/jamapsychiatry.2020.0322
19. Amiri S, Mahmood N, Mustafa H, Javaid SF, Khan MA. Occupational risk factors for burnout syndrome among healthcare professionals: a global systematic review and meta-analysis. Int J Environ Res Public Health. 2024;21(12):1583. https://doi.org/10.3390/ijerph21121583
